Vitamin D Treatment for COVID-19 Patients Nearly Erased Need for ICU Admission

From GrassrootsHealth
Early on in the COVID-19 pandemic, GrassrootsHealth, collaborated with Dr. William Grant and others, to publish a paper titled Evidence that Vitamin D Supplementation Could Reduce Risk of Influenza and COVID-19 Infections and Deaths on the relationship between vitamin D, immune function, and viral infections of the upper respiratory system. We have also shared a wealth information on the role of vitamin D in immune system health and function, and reviewed many studies that have demonstrated the association between vitamin D and improved outcomes for acute respiratory disorders, such as Acute Respiratory Distress Syndrome (ARDS).
Now that there has been time for the planning, execution, and analysis of several trials on vitamin D and COVID-19 outcomes, studies are now being published that provide direct evidence of the effect of vitamin D supplementation on COVID-19 patients, and the association of vitamin D intake and/or status on disease severity and death.
Recent Trial Shows Unique and Promising Results
 One of the latest studies on vitamin D and COVID-19, published by Castillo et al., enrolled 76 COVID-19 patients hospitalized with symptoms of acute respiratory infection and randomized them to the vitamin D treatment group (n=50) or the control group (n=26). There were 45 men and 31 women with an average age of 53 years. Their goal was to determine if early intervention with 25(OH)D, the metabolite of vitamin D used to measure vitamin D status, could improve outcomes of COVID-19 and reduce the need for Intensive Care Unit (ICU) admission.
One of the latest studies on vitamin D and COVID-19, published by Castillo et al., enrolled 76 COVID-19 patients hospitalized with symptoms of acute respiratory infection and randomized them to the vitamin D treatment group (n=50) or the control group (n=26). There were 45 men and 31 women with an average age of 53 years. Their goal was to determine if early intervention with 25(OH)D, the metabolite of vitamin D used to measure vitamin D status, could improve outcomes of COVID-19 and reduce the need for Intensive Care Unit (ICU) admission.
Both groups received the standard care for COVID-19, consisting of a combination treatment of hydroxychloroquine and azithromycin, with additional standard treatments as necessary. The vitamin D treatment group also received a .532 mg dose of oral calcifediol (25(OH)D) at admission, followed by .266 mg doses on days 3 and 7, and then once weekly until either discharged or admitted to the ICU. Calcifediol, or 25-hydroxyvitamin D3, was given due to its reliable intestinal absorption and to omit the need for hydroxylation of vitamin D3 to 25(OH)D in the liver, therefore leading to a more rapid improvement in 25(OH)D levels and availability.
What were the outcomes of this study?
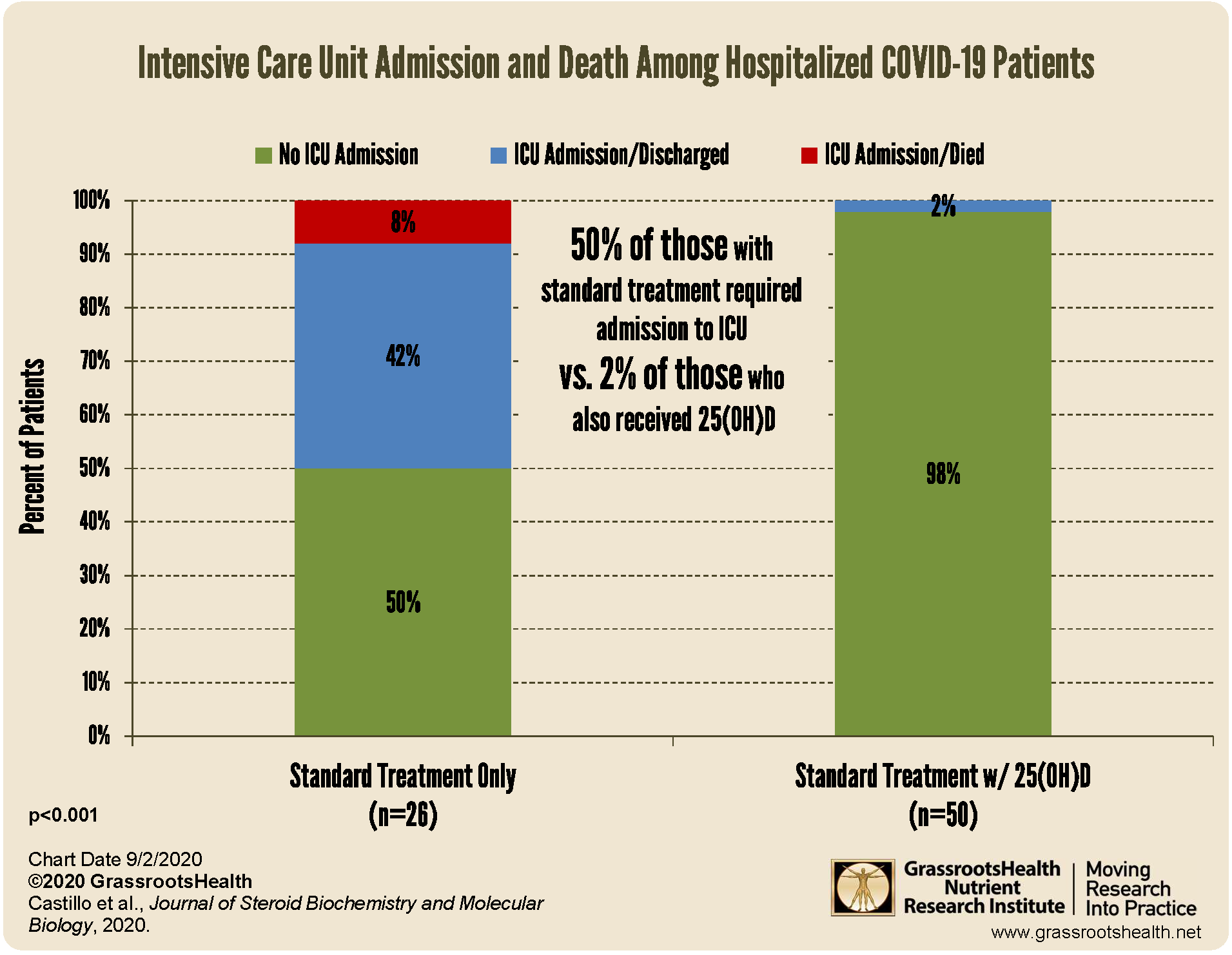
The study found that the administration of 25(OH)D at the early stages of COVID-19 significantly reduced the need for admission to the ICU, regardless of existing comorbidities, as illustrated in the chart below.
In fact, of the 26 patients in the control group, 13 (50%) required admission to the ICU with two resulting deaths, while only one patient out of the 50 (2%) in the vitamin D group required admission to the ICU, with no resulting deaths.
Click here to read more from GrassrootsHealth.
SmartTan.com news articles regularly report medical and scientific information to keep you abreast of current events related to UV light. This information is not intended to be used by any party to make unwarranted health claims to promote sunbed usage. Indoor tanning businesses are obligated to communicate a fair and balanced message to all clients about your products and services including the potential risks associated with indoor tanning. Contact your Smart Tan representative to find out more about what you can and can’t say in your tanning salon business.
© 2020 International Smart Tan Network. All rights reserved.